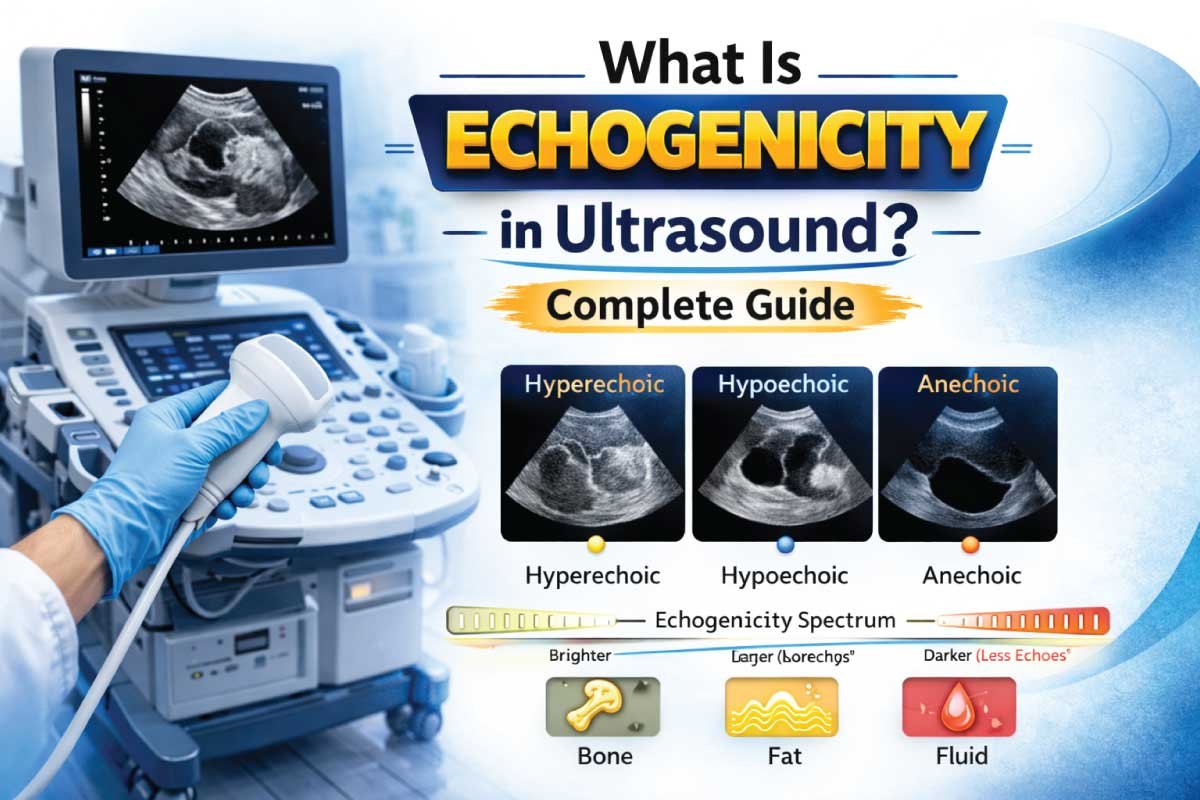
Echogenicity in ultrasound is a fundamental concept that describes how tissues reflect sound waves during an ultrasound examination. It determines how bright or dark a structure appears on a grayscale ultrasound image. Understanding echogenicity is essential for interpreting sonographic images, diagnosing medical conditions, and guiding procedures accurately.
Echogenicity is influenced by the tissue’s composition, density, and interface with surrounding structures. Different tissues produce varying echo intensities, resulting in hypoechoic, hyperechoic, anechoic, or isoechoic appearances. Clinicians use these differences to identify organs, lesions, fluid collections, and abnormalities in the body.
Basic Concept of Echogenicity
Echogenicity refers to the ability of a tissue to reflect ultrasound waves back to the transducer. Strongly reflective tissues produce brighter signals, whereas weakly reflective tissues produce darker signals. These differences form the grayscale images seen on ultrasound monitors.
The term “echogenic” comes from “echo,” indicating reflected sound waves, and “genic,” meaning producing. By assessing echogenicity, sonographers can distinguish normal tissues from pathological changes, evaluate fluid collections, and detect masses, cysts, or other abnormalities effectively.
How Echogenicity Works in Ultrasound
During an ultrasound scan, the transducer emits high-frequency sound waves that travel through tissues. When the waves encounter interfaces of different densities, a portion is reflected back as echoes, while the rest continues to deeper structures.
The returning echoes are analyzed by the ultrasound system:
- Strong echoes → bright appearance
- Weak echoes → dark appearance
- No echoes → black (anechoic)
This relationship allows clinicians to interpret structural and pathological differences in the tissues being scanned.
Types of Echogenicity
Echogenicity is categorized based on the intensity of echoes relative to surrounding tissues.
| Echogenicity | Appearance | Description | Example |
|---|---|---|---|
| Hyperechoic | Bright / White | High reflection, strong echoes | Bone, gallstones, calcifications |
| Hypoechoic | Dark Gray | Low reflection, weak echoes | Liver lesions, solid masses |
| Isoechoic | Similar to surrounding tissue | Same echogenicity as reference tissue | Normal liver parenchyma compared to spleen |
| Anechoic | Black | No echoes, fluid-filled | Simple cysts, urine in bladder |
| Heteroechoic | Mixed | Combination of echogenic patterns | Tumors, complex cysts |
These patterns help radiologists and sonographers differentiate normal anatomy from abnormal findings.
Factors Affecting Echogenicity
Several factors influence echogenicity, including:
-
Tissue composition – Fat, muscle, and fluid reflect sound differently.
-
Density differences – Interfaces between high- and low-density tissues generate stronger echoes.
-
Frequency of ultrasound – Higher frequencies improve resolution but may alter perceived echogenicity.
-
Angle of incidence – Perpendicular sound waves generate stronger echoes than oblique angles.
-
Pathological changes – Inflammation, fibrosis, or calcification can increase echogenicity.
These factors are essential for accurate interpretation of ultrasound images.
Clinical Applications of Echogenicity
Abdominal Ultrasound
Echogenicity is used to evaluate:
- Liver texture (fatty infiltration increases echogenicity)
- Kidney parenchyma (detect cysts or tumors)
- Spleen and pancreas (assessing normal vs abnormal tissue)
Changes in echogenicity help diagnose diseases like hepatitis, cirrhosis, and renal lesions.
Obstetric and Gynecologic Imaging
Echogenicity assists in:
- Fetal organ development assessment
- Placenta evaluation
- Detection of ovarian cysts or uterine fibroids
For example, anechoic amniotic fluid contrasts with echogenic fetal tissues, aiding visual clarity.
Musculoskeletal Imaging
Muscles, tendons, and ligaments have specific echogenic patterns:
- Tendons appear hyperechoic with fibrillar patterns
- Muscles are hypoechoic with linear striations
- Fluid collections are anechoic
These patterns guide diagnosis of tears, inflammation, or hematomas.
Cardiac Ultrasound
Echogenicity is critical in echocardiography to:
- Differentiate myocardium from blood
- Visualize valves (hyperechoic)
- Detect calcifications or thrombi
Proper evaluation of echogenicity helps assess cardiac function and identify pathological changes.
Importance of Echogenicity in Pathology
Changes in echogenicity often indicate disease:
- Increased echogenicity → fibrosis, calcifications, fatty infiltration
- Decreased echogenicity → edema, inflammation, cystic degeneration
- Mixed echogenicity → complex masses or tumors
By comparing echogenicity with surrounding tissues, clinicians can classify lesions, determine severity, and plan treatment.
Echogenicity in Ultrasound-Guided Procedures
During interventions like biopsies or drainages, echogenicity:
- Helps identify target lesions
- Guides needle placement
- Confirms needle position relative to hyperechoic or hypoechoic areas
This improves safety, precision, and success rates of ultrasound-guided procedures.
Read More:
Quantitative vs Qualitative Echogenicity
Echogenicity can be evaluated in two ways:
Qualitative
- Visual assessment of brightness patterns
- Compares tissue to surrounding structures
- Subjective, relies on operator experience
Quantitative
- Uses software to measure pixel intensity
- Provides numerical echogenicity values
- Useful for monitoring changes over time (e.g., liver fibrosis)
Both methods are important in clinical practice.
Echogenicity and Doppler Ultrasound
Doppler ultrasound complements echogenicity by assessing blood flow, while echogenicity provides tissue characteristics.
- Hypoechoic areas may indicate vessels or fluid collections
- Hyperechoic areas may represent calcified plaques
- Doppler helps confirm vascularity or obstruction
This combination enhances diagnostic accuracy in vascular and organ imaging.
Advantages of Understanding Echogenicity
| Advantage | Explanation |
|---|---|
| Accurate diagnosis | Differentiates normal from abnormal tissues |
| Non-invasive | Provides detailed tissue information without radiation |
| Real-time assessment | Immediate evaluation of organs and lesions |
| Procedure guidance | Assists biopsies, drainages, and injections |
| Disease monitoring | Quantitative echogenicity tracks progression |
Echogenicity is a key parameter for clinical decision-making in ultrasound imaging.
Limitations of Echogenicity
| Limitation | Reason |
|---|---|
| Operator dependent | Requires experience to interpret correctly |
| Subjective variations | Visual assessment may differ between sonographers |
| Limited specificity | Echogenicity changes can be non-specific |
| Poor visualization through bone or gas | Structures behind bone or air may be obscured |
Despite these limitations, echogenicity remains crucial for accurate sonographic interpretation.
Read More:
Echogenicity in Different Organs
Liver
- Normal liver is homogeneous and moderately echogenic
- Increased echogenicity → fatty liver
- Decreased echogenicity → inflammation, edema
Kidney
- Cortex is hypoechoic, medulla varies
- Increased echogenicity → chronic renal disease
- Anechoic areas → cysts or fluid collections
Thyroid
- Homogeneous, hyperechoic relative to surrounding muscles
- Nodules can be hypoechoic, hyperechoic, or mixed
Breast
- Fatty tissue is hypoechoic
- Glandular tissue is moderately echogenic
- Tumors often appear hypoechoic or heterogeneous
Techniques to Enhance Echogenicity Assessment
-
Adjusting gain – Controls image brightness
-
Proper frequency selection – Higher frequencies for superficial structures
-
Optimal transducer positioning – Reduces artifacts
-
Comparative scanning – Compare with contralateral or adjacent tissues
-
Use of harmonics – Improves contrast and tissue differentiation
These techniques improve accuracy and diagnostic confidence.
Read More:
Future of Echogenicity in Ultrasound
-
AI-assisted echogenicity quantification – Reduces operator dependency
-
3D and 4D echogenicity mapping – Enhanced spatial assessment
-
Integration with elastography – Combines tissue stiffness with echogenicity
-
Longitudinal studies – Monitor disease progression using quantitative data
Future advancements will make echogenicity more precise and standardized, enhancing patient care.
Conclusion
Echogenicity in ultrasound is a vital concept that describes tissue reflectivity and determines grayscale appearance. Understanding it allows clinicians to differentiate normal from abnormal tissue, detect lesions, and guide interventions safely.
From abdominal and cardiac imaging to musculoskeletal and obstetric applications, echogenicity helps identify pathology, monitor disease, and plan treatments. Quantitative and qualitative assessments, along with modern software and AI integration, ensure accurate and reproducible results.
By mastering echogenicity, sonographers can enhance diagnostic accuracy, guide procedures effectively, and provide high-quality patient care across diverse clinical specialties. It is the cornerstone of ultrasound interpretation and remains essential in modern medical imaging.

Zak is a dedicated medical and career writer specializing in sonography, healthcare education, and professional development. Through SonographerSalary.com, he shares in-depth insights on sonographer salaries, education pathways, and career tips to help readers build successful futures in medical imaging. His content combines accuracy with practical, easy-to-understand guidance, empowering students and professionals to make confident, informed career decisions.